Last Updated: 21 September, 2015
1.0 Introduction
 Diastasis recti is an anatomical term describing an acquired condition in which the right and left rectus muscles (think six-pack) have separated. The fascia (or covering) has become stretched, most often due to body habitus or pregnancy. Diastasis recti do not represent an abdominal wall hernia; there is no fascial defect and therefore, no risk of incarceration or strangulation.
Diastasis recti is an anatomical term describing an acquired condition in which the right and left rectus muscles (think six-pack) have separated. The fascia (or covering) has become stretched, most often due to body habitus or pregnancy. Diastasis recti do not represent an abdominal wall hernia; there is no fascial defect and therefore, no risk of incarceration or strangulation.
Although diastasis recti can occur in both genders and across age groups, it is principally seen in pregnant women. The condition impacts on body aesthetics and may be associated with stomach protrusion, hernia formation, lower back pain and impaired posture.
Section Two of this overview will provide the reader with a definition of diastasis recti, other common terms by which it is known, as well as defining some important terms. Section Three will then provide a description of the abdomen, particularly the muscles involved. Section Four will outline the causes of diastasis recti, why it is a problem and some of the known complications. Section Five will describe who can be affected by the condition and Section Six the prevalence and risk factors, as well as highlighting some of the inaccuracies across the studies. Section Seven will look at the symptoms across the identified populations affected by the condition before Section Eight describes how the condition is diagnosed and measured. Section Nine outlines some of the conditions which are similar to diastasis recti which the reader should be wary of. Section Ten provides a comprehensive overview of the treatments available such as physiotherapy, exercise and surgical interventions, as well as providing some general advice. Nearing the end, Section Eleven highlights the outlook for people with the condition. In the penultimate section, Section Twelve, the article lists some personal notes and finally, Section Thirteen provides a summary of the article.
2.0 What is Diastasis Recti?
Diastasis recti can be defined as:
“…a condition in which the medial borders of the rectus muscles slowly spread apart with thinning and stretching of the rectus sheath, resulting in a diffuse bulge in the upper midline abdomen.” (Norton, 2003, p.350).
Although precise definitions vary between researchers, the central premise that diastasis recti is an impairment characterised by a separation between the left and right side of the rectus abdominis muscles which covers the front surface of the belly area is consistent.
Figure 1: Diastasis recti (normal and gap)
The distance of separation, known as the inter-recti distance or IRD (Liaw et al., 2011), is created by the stretching of the linea alba[1], a connective collagen sheath created by the aponeurosis[2] (or tendon) insertions of the transverse abdominis, internal oblique, and external oblique (Brauman, 2008).
The condition is considered an abdominal protrusion (due to an abdominal wall weakness or defect) and therefore individuals should be aware of the differential diagnoses available (Section 9.0).
The wisdom in the medical literature consistently states that the condition of diastasis recti presents as a weakness or laxity of the abdominal wall, including the linea alba, but does not constitute a true hernia[3] as there is no fascial[4] defect and therefore no risk of incarceration or strangulation, and as a result is of no clinical significance.
2.1 Other Terms for Diastasis Recti
Diastasis recti is known by a variety of terms, as highlighted below:
- Abdominal Separation;
- Abdominal Muscle Separation;
- Rectus Diastasis (RD);
- Rectus Abdominis Diastasis (RAD);
- Diastasis of Rectus Abdominal Muscle (DRAM);
- Divarication of Rectus Abdominal Muscles (DRAM);
- Divarication of the Recti;
- Diastasis Rectus Abdominis (DRA);
- Abdominal Rectus Muscle Diastasis (ARD); or
- Abdominal Rectus Diastasis (ARD).
For the purposes of this article the term diastasis recti is used throughout to avoid confusion.
2.2 Defining the Terms
- Diastasis (Noun): An abnormal separation of parts normally joined together.
- Divaricate (Transitive Verb): To spread apart.
- Rectus (Noun): Any of several straight muscles.
- Recti: Plural of rectus.
- Rectus Abdominis: Is a long flat muscle that extends bilaterally along the entire length of the front of the abdomen. The rectus muscles acting together serve to bend the trunk forwards; acting separately they bend the body sideways.
- Linea Alba: A fibrous band that runs vertically along the centre of the anterior abdominal wall (between the two rectus muscles) and receives the attachments of the (internal and external) oblique and transverse abdominal muscles (Brauman, 2008). It contains the umbilicus (navel) and is also known as the white line or Hunter’s line.
- Parturition (Noun): The action or process of giving birth to offspring.
- Antepartum (Adjective): Relating to the period before parturition.
- Postpartum (Adjective): Occurring in or being the period following parturition.
- Antenatal (Adjective): Concerned with the care and treatment of the unborn child and of pregnant women.
- Postnatal (Adjective): Occurring or being after birth; specifically: of or relating to an infant immediately after birth.
- Prenatal (Adjective): Occurring, existing, performed or used before birth.
- Intranatal (Adjective): Occurring chiefly with reference to the child during the act of birth.
- Neonatal (Adjective): Of, relating to, or affecting the newborn and especially the human infant during the first month after birth.
- Plication (Noun): The tightening of stretched or weakened bodily tissues or channels by folding the excess in tucks and suturing (stitching).
- Aponeurosis (i.e. Tendons) (Noun): Any of the broad flat sheets of dense fibrous collagenous connective tissue that cover, invest, and form the terminations and attachments of various muscles.
3.0 Anatomy of the Abdomen
The anterior abdominal wall consists of three layers (Figure 2) of flat muscles, the tendons (aponeuroses) of which interlace in the midline, and a vertically orientated pair of segmented muscles which are en-sheathed incompletely by the aponeuroses of the three flat muscles (sheath of the rectus abdominis). The flat muscles arise from the lateral aspect of the torso (inguinal ligament, iliac crest, thoracolumbar fascia, lower costal cartilages and ribs). The lowest fibres of external oblique roll inwardly to form the inguinal ligament. These three muscles act to compress the abdominal contents during expiration, urination and defecation. They assist in maintaining pressure on the curve of the low back, resisting ‘sway back’ (excess lumber lordosis[5]) and extension of the low back.
Figure 2: 3 Layers of the Anterior Abdominal Wall (Source: Kapit & Elson, 1993, p.43)
Each segmented rectus abdominis muscle arises from the pubic crest and tubercles, and inserts on the lower costal cartilages and xiphoid process (sternum). They are flexors of the vertebral column. The sheath of the rectus varies in its extent, running from deep to superficial from below upward, as illustrated in Figure 2 (Deep Layer). Below the arcuate line[6][7], no muscle contributes to its posterior layer (E2*); in the middle, all three flat muscles contribute equally to the sheath (E1*); above, the anterior sheath is formed from external oblique; posteriorly, the rectus contacts the costal cartilages.
The inguinal region is the lower medial portion of the abdominal wall. Herein exists the inguinal canal with its inner (deep inguinal ring) and outer (superficial inguinal ring) openings, and the resident spermatic cord (ductus deferens and testicular vessels and nerves) in the male and the round ligament of the uterus in the female. In its apparent ‘migration’ from the abdominal cavity through the inguinal canal into the scrotum during the last months of foetal development, the testis and spermatic cord push through (not perforate) and carry with them each layer of abdominal wall they traverse, much as a finger might push through four layers of latex to form a four-layered finger glove. Each of these layers constitutes a covering of the cord. The inguinal canal is a site of relative structural weakness in both males and females, and the abdominal wall here is subject to protrusions (inguinal hernia) from intra-abdominal fat and intestines, indirectly through the deep ring or directly through the wall near the superficial ring.
4.0 What Can Cause Diastasis Recti?
Diastasis recti can be caused by (Emanuelsson, 2014):
- Pregnancy, due to:
- Fluctuations in weight during pregnancy.
- Increased intra-abdominal pressure.
- Hormonal changes combined with uterine growth.
- Caesarean section (possibly due to changes in anatomical morphology of the abdominal wall after caesarean section).
- Genetic variations in collagen composition (e.g. connective tissue disorders).
- Hereditary factors.
- Massive weight loss occurring spontaneously or after bariatric surgery.
- Previous abdominal surgery.
4.1 Why Is It A Problem?
Those affected by diastasis recti should be as equally concerned about the functional issues of having the condition as they are about the cosmetic issues; although the functional aspects will have a greater impact on their daily activities. Muscles, particularly those of the abdomen (the obliques, transversus, and recti) provide dynamic stability and fine control to the spine (Speed, 2004).
When the rectus muscles are no longer attached to each other in the linea alba or midline, they no longer contract effectively. The upper arms and trunk do work, and need to push off against a pressurised abdomen. With diastasis recti, a lack of coordinated muscle contraction and the expanded size of the abdominal cavity works against effectively raising intra-abdominal pressure.
When conducting activities such as going up stairs, exercise, or other acts of daily living, a diastasis recti causes other parts of the body, such as the back, to work harder. Therefore, repair of the diastasis recti (through manual therapy or surgery) often gives patients better use of the torso, and often improves mild lower back pain if it is present.
4.2 What Are The Complications?
It is important to note that this condition has no associated morbidity[8] or mortality[9] (Norton, 2003). In general, complications only result when a hernia develops, as diastasis recti is generally asymptomatic.
In contrast to epigastric hernias, diastasis recti is not a fascial defect or hernia per se, and consequently presents no threat of complication or strangulation (Akram & Matzen, 2014); diastasis recti is merely a cosmetic deformity (Norton, 2003).
Some researchers suggest that failure to treat diastasis recti successfully can lead to long term sequelae[10] (Candido et al., 2005), including:
- Abnormal posture (Boissonault & Blaschak, 1988);
- Lumbo-pelvic pain (Candido et al., 2005; Parker et al., 2009), although Mota et al. (2014, p.204) state that “Women with [diastasis recti] were not more likely to report lumbo-pelvic pain than women without [diastasis recti].”;
- Cosmetic defects (Candido et al., 2005);
- Psychological discomfort (i.e. body image);
- Physical discomfort such as low back pain (Emanuelsson, 2014);
- Corset instability;
- Poor postural stability (Emanuelsson, 2014);
- Bulging of the abdominal wall (Emanuelsson, 2014;
- Swelling after food intake (Emanuelsson, 2014);
- Abdominal wall weakness and reduced muscular abdominal strength (Emanuelsson, 2014); and/or
- Limitations during physical activity (Emanuelsson, 2014).
- View Section 10.4 for surgical complications.
In addition, a diastasis recti can change the appearance of the abdomen. The skin may droop, and some patients may even develop an actual hernia through the midline. Also, some postpartum patients may complain of continuing to look pregnant.
There is a general consensus that medical professionals (aimed at general practitioners rather than surgeons) may not take diastasis recti seriously as the functional impact on health is not understood. Diastasis recti does not lead to emergency conditions such as herniation of abdominal contents, but symptoms can develop in the long-term perspective due to weakening of the abdominal wall and the pelvic girdle.
5.0 Who Can Be Affected By Diastasis Recti?
Although diastasis recti can occur in both genders and across age groups, it is principally seen in pregnant women. Populations affected include:
- Female Population: Diastasis recti is common in post-partum women (Akram & Matzen, 2014). In pregnant or postpartum women, the condition is caused by the stretching of the rectus abdominis by the growing uterus (the abdominal muscles and ligaments stretch throughout pregnancy under the influence of the hormones Progesterone and Relaxin). It is more common in multiparous women due to repeated episodes of stretching. When the condition occurs during pregnancy, the uterus can sometimes be seen bulging through the abdominal wall beneath the skin.
- Newborn Population: In the newborn, the rectus abdominis is not fully developed and may not be sealed together at the midline. However, this typically resolves on its own.
- Infant Population: It is often present in young children due to lack of strength of the linea alba (Uffman, 2012).
- Male Population.
- Other Populations: “Seen most commonly in obese middle-aged and poorly conditioned individuals, especially when they raise their heads while laying supine” (AHC Media, 2014).
6.0 Prevalence and Risk Factors
According to Mota and Colleagues (2015) there is scant knowledge on both prevalence and risk factors for the development of diastasis recti; although this is slightly contradicted by their earlier research (Mota et al., 2014). Emanuelsson (2014, p.5) also states that “no reliable data exist regarding evaluation of patients with diastasis recti prior to surgery and the relevance of specific symptoms, width of diastasis and abdominal wall strength.”
Nonetheless, there is research, mainly from the late 1980s and 1990s, which provides insight in to both prevalence and risk factors. This research suggests that diastasis recti:
- May affect between 30%-70% of pregnant women (Boissonnault & Blaschak, 1988), and between 66 and 100% of women in the third trimester of pregnancy (Boissonault & Blaschak, 1988; Candido et al., 2005).
- Transient diastasis recti: it is not uncommon for women to experience muscle separation during the third trimester of pregnancy or the immediate postpartum period, and is a normal physiological event that usually reverts spontaneously.
- Permanent diastasis recti: is less frequent at 10-15% and most often occurs in women who have been pregnant three or more times or have carried large babies. The condition is thought to be caused by the accumulated effects of maternal hormones (which relax abdominal muscles and soften connective tissues) and the repeated biomechanical stretching of the abdominal wall.
- May remain separated in the immediate postpartum period in 35%-60% of women (Bursch, 1987); Mota et al. (2014) recorded 39% of women at 6 months postpartum. Mota et al. (2014) did not identify any risk factors for women with diastasis recti at 6 months postpartum in their study.
- Can be found in 39% of older, parous[11] women undergoing abdominal hysterectomy (Ranney, 1990). Among 1738 parous women who needed abdominal hysterectomies, 553 were found to have mild, 108 had moderate, and 12 had severe diastasis recti, several years postpartum (Ranney, 1990).
- Can be found in 52% of urogynaecological menopausal patients (Spitznagle et al., 2007).
Other factors include:
- Age (Emanuelsson, 2014), women over the age of 35 (Lo et al., 1999; Harms, 2014);
- High birth weight of child (Harms, 2014);
- Multiple birth pregnancy (Lo et al., 1999; Harms, 2014);
- Multiple pregnancies (Harms, 2014);
- Caesarean section (Lo et al., 1999; Emanuelsson, 2014);
- Excessive abdominal exercises after the first trimester of pregnancy (Harms, 2014);
- Massive weight loss occurring spontaneously or after bariatric surgery (Emanuelsson, 2014);
- Previous or repeated abdominal surgery (Emanuelsson ,2014);
- Hereditary disorders and genetic factors (Emanuelsson, 2014); and
- Abdominal Aortic Aneurysm (AAA): the prevalence of diastasis recti in men “is approximately twice as high in patients with [AAA] than in those without.” (De’Ath et al., 2010, p.593), and AAA patients also had a higher median body mass index (BMI).
Emanuelsson (2014) suggests that the width of the linea alba seems to be more dependent on age than on BMI, and that the impact of BMI is dependent on whether or not there is an increase in the amount of intra- or extra-abdominal fat.
VoxHealth provides some interesting demographics and statistics on diastasis recti, which it claims are based on anonymised patient records.
6.1 Men
There is currently no data in the literature on the incidence of diastasis recti in men (Emanuelsson, 2014). However, research published by Lockwood (1998) suggests there may be a history of weight fluctuations, weightlifting, or full-excursion sit-up exercises, which may lead to progressive separation of the rectus muscles over time. Other aetiological factors include chronic or intermittent abdominal distension, advancing age, or familial weakness of the abdominal musculofascial tissues (Lockwood, 1998).
6.2 Newborns and Infants
Newborns and infants may suffer from diastasis recti because the abdominal muscles may not have matured enough to close the gap between the two halves. The ridge between the muscles is most noticeable when the infant sits up, as using the muscles forces them to contract, accentuating the ridge. As the newborn/infant grows, the two halves grow closer together, and the diastasis recti gradually becomes smaller, until it disappears. Therefore, surgery is seldom needed to repair the gap between the two halves of the rectus abdominis. The only time it may be necessary is if the newborn/infant develops a hernia, which may become trapped in the space between the two halves and prevent them from closing properly.
There is a perennial view across the various websites that discuss diastasis recti that the condition “is more common in premature and African American newborns” (Kuber, 2013, p.48). Brown and Miller (2005, p.92) state the same in their book. However, no studies or research have been found that substantiates these claims; except for Spitnagle et al. (2006, p323). Strangely, the sentence quoted above, in its exact form, is repeated on all the websites encountered during the research for this article!
6.3 Inaccuracy across Studies
When looking at the literature the reader must be wary of inaccuracy due to:
- Different cut off points for diagnosis (Bursch, 1987; Boissonault & laschak, 1988; Gilleard & Brown, 1996; Rath et al., 1996; Chiarello et al., 2005; Spitznagel et al., 2007; Beer et al., 2009);
- Use of different measurement methods;
- Most prevalence studies being based on palpation (Bursch, 1987; Boissonault & Blaschak, 1988; Mantle et al., 2004) or calipers (Boxer & Jones, 1997; Hsia & Jones, 2000) which may be less reliable than ultrasonography (Mota el al., 2013);
- Few studies about the ‘normal’ width of IRD in women (Coldron et al., 2008; Liaw et al., 2011); and
- Scant knowledge about risk factors (Benjamin et al., 2014).
7.0 What are the Symptoms?
7.1 In General
A diastasis recti looks like a ridge, which runs down the middle of the belly area, stretching from the bottom of the breastbone to the belly button (midline of the abdomen, anywhere from the xiphoid process to the umbilicus).
It becomes more prominent with straining and may disappear when the abdominal muscles are relaxed. The medial borders of the right and left halves of the muscle may be palpated during contraction of the rectus abdominis.
7.2 For Newborns
May appear as a ‘bubble’ or ‘ridge’ running down the abdomen from the xiphoid process to the umbilicus. It is more prominent with increased intra-abdominal pressure.
7.3 For Infants
 The linea alba is often wide and lax in infants and young children, so when they strain, the midline fascia bulges forward, sometimes quite dramatically (Zaoutis & Chiang, 2007). This minor defect may allow tissue from inside the abdomen to herniate anteriorly. On infants, this may manifest as an apparent ‘bubble’ under the skin of the belly between the umbilicus and xiphisternum[12].
The linea alba is often wide and lax in infants and young children, so when they strain, the midline fascia bulges forward, sometimes quite dramatically (Zaoutis & Chiang, 2007). This minor defect may allow tissue from inside the abdomen to herniate anteriorly. On infants, this may manifest as an apparent ‘bubble’ under the skin of the belly between the umbilicus and xiphisternum[12].
- It is most easily seen when the infant tries to sit up.
- When the infant is relaxed, you can often feel the edges of the rectus muscles.
“This is a self-correcting anatomic variant that does not require surgical therapy.” (Zaoutis & Chiang, 2007, p.891).
7.4 During Pregnancy
 Most women do not complain of pain when diastasis recti occurs. However, they may notice bulging in their abdominals when using these muscles, for example when:
Most women do not complain of pain when diastasis recti occurs. However, they may notice bulging in their abdominals when using these muscles, for example when:
- Sitting up in bed;
- Coughing;
- Laughing; and/or
- Getting out of the bath.
A small percentage of women may have pain when the diastasis recti is quite large, this may be in the (lower) back or within the abdominals. It is commonly seen in women who have multiple pregnancies, because the muscles have been stretched many times. Extra skin and soft tissue in the front of the abdominal wall may be the only signs of this condition in early pregnancy. In the latter part of pregnancy, the top of the pregnant uterus is often seen bulging out of the abdominal wall. An outline of parts of the unborn baby may be seen in some severe cases.
7.5 During Exercise
Individuals with diastasis recti usually perceive no pain at rest whereas discomfort, pain, corset instability and bulging of the abdominal wall are symptoms appearing during physical activity (Emanuelsson, 2014).
If an individual is diagnosed with or suspects a diastasis recti they should avoid the following activities as they can exacerbate the condition:
- Abdominal sit-ups;
- Crunches;
- Oblique curls;
- Double leg lifts;
- Upper body twisting exercises;
- Exercises that include backbends over an exercise ball;
- Yoga postures that stretch the abs, such as ‘cow pose’ or ‘up-dog pose’;
- Pilates exercises that require the head to be lifted off the floor;
- Lifting and carrying heavy objects;
- Intense coughing without abdominal support;
Individuals will need to avoid any exercise that causes their abdominal wall to bulge out upon exertion. Once the diastasis recti has ‘closed’ or, perhaps more accurately, narrowed to a ‘more normal’ distance, then individuals can gradually add these activities back in.
8.0 How is it Diagnosed/Measured?
Diastasis recti should only be diagnosed by a medical professional (i.e. a physiotherapist, midwife or medical doctor) who will check for the condition by feeling the abdomen. If suspected, a midwife or doctor may refer for physiotherapy.
With this in mind, distasis recti can be diagnosed/measured through one of four methods:
- Abdominal palpation (Boissonnault & Blaschak, 1988);
- Calipers: dial and digital (Hsia & Jones, 2000; Chiarello & McAuley, 2013);
- Ultrasound measurement (Mota et al., 2013); or
- Computed Tomography (CT) Scanning (Emanuelsson, 2014).
The diagnosis of diastasis recti is often made when a patient, in the supine position, attempts to raise their head during an examination. The increase in intra-abdominal pressure, as the two rectus muscles contract, causes a diffused fusiform[13] bulge through the thin midline fascia (Stevens, 2013).
8.1 Classification
The criteria for the diagnosis of diastasis recti varies and the literature suggests that abnormal separation exists between the right and left rectus abdominis muscles when the IRD exceeds 1.5 cm (Engelhardt, 1998; Gilleard & Brown, 1996), 2 cm (Potter et al., 1997; Lo et al., 1999), 2.5 cm (Candido et al., 2005) or 2.7 cm or greater (Benjamin et al., 2014) when measured in a lying position at rest; or greater than 2 fingers width when measured in a crook lying position (Bursch, 1987; Sheppard, 1996).
However, the general definition of a ‘normal’ linea alba is generally accepted as a width of 15 mm at the xiphoid process, 22 mm at 3 cm above the umbilicus, and 16 mm at 2 cm below the umbilicus (Beer et al., 2009).
Another study including 40 cadavers and 40 abdominal-pelvic scans suggested that the width of the linea alba is age dependent. Furthermore, data indicated that in women younger than 45 years the linea alba was 10 mm at the supra-umbilical level, 27 mm at the umbilicus, and 9 mm between the pubic symphysis and umbilicus. Corresponding values in women older than 45 years were 15, 27 and 14 mm respectively (Rath et al., 1996).
Emanuelsson (2014) suggests that several aetiological factors may lead to protrusion of the anterior abdominal wall. Also, it has not been studied whether diastasis recti is an entity in itself or should be seen as part of a complex aponeurotic system of the entire anterior and lateral abdominal wall. A specific classification based on different myoaponeurotic deformities has been introduced (Nahas, 2001), which are defined as:
- Type A: Women presenting with diastasis recti after pregnancy.
- Type B: Laxity of the lateral and inferior parts of the anterior abdominal wall.
- Type C: Lateral insertion of the rectus muscles to lateral costal cartilages.
- Type D: A poor waistline.
Nahas’ classification is a general description of anterior abdominal wall weakness without specific focus on diastasis recti; despite this it has gained some popularity amongst clinicians (Emanuelsson, 2014).
8.2 Abdominal Palpation
Examination is performed with the subject lying on their back, knees bent at 90° with feet flat, head slightly lifted placing chin on chest. With muscles tense, examiners then place fingers in the ridge that is presented. Measurement of the width of separation is determined by the number of fingertips that can fit within the space between the left and right rectus abdominis muscles (Engelhardt, 1988).
8.3 Calipers
Instead of fingertips, the calipers (dial or digital) measure the gap in millimetres.
8.4 Ultrasound Measurement
Ultrasound investigation is another method described in the literature, but it is highly dependent on the skills of the examiner (Mendes et al., 2007). Further, Emanuelsson (2014, p.43) states “The ultrasound transducer is available with a 4-6 cm field width, which limits the field of view during measurement and may have impact on the accuracy of the examination.”
Mota et al. (2013) suggest that although palpation has sufficient reliability to be used in clinical practice, ultrasound is a more accurate and valid method. This was due to ultrasound measures being highly sensitive to changes of IRD, which is not possible to replicate by palpation assessment using a finger width scale.
8.5 Computed Tomography (CT) Scanning
CT scanning, a highly specific method, can be used to provide a radiologic assessment of the width of the diastasis recti, although it would appear to underestimate the width of diastasis recti (Emanuelsson, 2014). Part of the problem is that CT scanning will identify the most medially located muscle fibres of the rectus muscles that have no relevance for muscular activity, thus leading to underestimation of diastasis recti width (Emanuelsson, 2014).
Further, CT scanning is time-consuming, expensive and exposes patients to radiation, but was considered the gold standard for the assessment of diastasis recti at the beginning of Emanulsson’s study (Mendes et al., 2007; Mota et al., 2012).
Accordingly, Emanuelsson (2014, p.43) suggests that “preoperative clinical measurement” is the most effective way of measuring diastasis recti width prior to “clinical decision making”.
9.0 Differential Diagnosis
As noted in the previous section there are a number of methods to diagnose diastasis recti, however, there are a variety of ailments which have similar symptoms which the reader should be aware of. Conditions that weaken the abdominal wall are often associated with stomach protrusion, hernia development and contour abnormalities.
9.1 Hernias (In General)
Diastasis recti can be distinguished from incisional, congenital and acquired midline hernias of the abdominal wall. While a true hernia is associated with a fascial defect, patients with diastasis recti have no detectable fascial defect when they are supine (Stevens, 2013). Further, diastasis recti “must be differentiated from an epigastric hernia or incisional hernia, if the patient has had abdominal surgery” (Norton, 2003, p.350). Hernias may be ruled out using ultrasound.
9.2 Epigastric Hernias
Epigastric hernias arise in the upper abdomen along the linea alba, and usually appears in adulthood, often in association with obesity or pregnancy. Epigastric hernias frequently present as small defects (small bulges within the prominent ridge) with incarcerated pre-peritoneal[14] fat or omentum[15], causing pain and warranting repair (Uffman, 2012). Diastasis recti is a condition in which the medial borders of the rectus muscles slowly spread apart with thinning and stretching of the rectus sheath, resulting in a diffuse bulge in the upper midline abdomen. In contrast to epigastric hernias, diastasis recti is not a fascial defect or hernia per se, and consequently presents no threat of complication; diastasis recti is merely a cosmetic deformity.
Underlying epigastric hernias should be ruled out and ultrasound may be helpful if an epigastric hernia is suspected (Uffman, 2012). In the absence of an epigastric hernia, no surgical repair is required (Uffman, 2012).
9.3 Abdominal Protrusion
Abdominal protrusion can be a result of multiple factors including:
- Extra-abdominal fat;
- Intra-abdominal fat;
- Diastasis recti;
- Abdominal wall hernia; and
- Global myofascial laxity.
10.0 Treatment
Conclusive data regarding the most appropriate treatment of diastasis recti are sparse, and studies with focus on abdominal wall function and quality of life after repair are lacking. Furthermore, no reliable data exist regarding evaluation of patients with diastasis recti prior to surgery and the relevance of specific symptoms, width of diastasis and abdominal wall strength (Emanuelsson, 2014).
Prior to 2014 no information existed in the literature about the effect of abdominal muscle contraction on the IRD distance in postpartum women. This absence did not discourage individuals (mainly physiotherapists and fitness professionals) from recommending abdominal muscle strengthening exercises during the postpartum period, particularly to reduce the IRD (Benjamin et al., 2014).
A systematic review of the evidence by Benjamin et al. (2014) found that exercise may or may not reduce the size of the gap in pregnant or postpartum women. The authors looked at 8 studies totalling 336 women and concluded that “Due to the low number and quality of included articles there was insufficient evidence to recommend that exercise may help to prevent or reduce diastasis recti. (Benjamin et al., 2014). However, Akram and Matzen (2014) concluded that antepartum activity level may have a protective effect on diastasis recti and exercise may improve post-partum symptoms of diastasis recti. Further, a study by Pascoal and Colleagues (2014) suggests that isometric contractions can reduce the IRD in postpartum women.
Research for this article suggests there are a number of generally accepted common elements in the treatment process for diastasis recti which include:
- Proper fitting for an abdominal brace, if needed;
- Core stabilisation exercises;
- Postural training;
- Education and training on appropriate mobility techniques; and
- Education and training on appropriate lifting techniques.
For some cases a self-guided programme may be enough to correct a diastasis recti. However, it is recommended that postpartum women and post-surgical patients see a qualified pelvic floor physiotherapist if they believe they have a diastasis recti. Patients with diastasis recti may have co-morbidities (i.e. other things going on), and a pelvic floor physiotherapist will evaluate everything from the ribs down to the knees. Elements that a physiotherapist may assess/examine include:
- Assessment of the length and width of the separation;
- Examine strength of the patient’s transverse abdominis muscle;
- Assess motor control of the pelvic floor;
- Postural assessment (sitting and standing); and
- (Possibly) assessment of hip, back and sacral stability.
Knowing a patient’s overall ‘impairments’ is important in the treatment process of diastasis recti, because only then can an appropriate treatment plan be developed. Since every patient is different, treatment plans should be specifically tailored for each patient.
10.1 General Advice
- Avoid heavy lifting. Where you have to lift please do so correctly by keeping your back straight and bending your knees.
- Avoid movements which may prevent the separation recovering, such as sitting straight up when getting out of the bath or bed and/or heavy lifting.
- When getting out of bed, roll onto your side first with knees bent, then pull in your lower abdominal muscles as you place your legs over the side of the bed and push yourself up into sitting with your arms. Reverse the process to get back into bed.
- Support your stomach during any activities that increase pressure within the stomach, e.g. sneezing, coughing and laughing to prevent it from bulging and the gap becoming worse.
- Physiotherapists may fit some elasticated abdominal support in order to encourage the linea alba to recover.
- Avoid any exercises, which cause the stomach to bulge e.g. sit-ups. Discuss suitable exercises with your physiotherapist.
- After the birth of a baby, the abdominal muscles will feel weak and stretched. As Relaxin and Progesterone will now start reducing, the muscles and ligaments will again become toned.
- No (medical) treatment is necessary for women while they are still pregnant.
- Typically, the separation of the abdominal muscles will lessen within the first 8 weeks after childbirth. However, the connective tissue remains stretched for many postpartum women. The weakening of the abdominal muscles and the reduced force transmission from the stretched linea alba may also make it difficult to lift objects, and cause lower back pain. Additional complications can manifest in weakened pelvic alignment and altered posture.
- Surgery may be needed if the newborn [baby] develops a hernia that becomes trapped in the space between the muscles.
- In infants, complications include development of an umbilical or ventral hernia, which is rare and can be corrected with surgery. In infants, the rectus abdominis muscles continue to develop and the diastasis recti will disappear over time.
- Ensure that your diastasis recti has decreased to at least two finger widths before starting to gradually return to other activities and more challenging exercises, usually from around three months postnatal.
- Recovery time, after childbirth, can vary and it is important to be patient and persevere with the exercises and advice.
- If you feel you are not improving, or your diastasis recti is very large, ask your general practitioner (GP) for a referral to a Women’s Health Physiotherapist.
- Physiotherapists, and personal trainers, should be able to help as long as they are current with the latest research for training of the postpartum abdominal wall and are familiar with what to look for when training individuals with diastasis recti.
10.2 Physiotherapy
Firstly, the profession of physiotherapist (aka physical therapists) does not have one standard guideline on what moves/exercises will bring the belly muscles back into line. Secondly, physiotherapy treatment is available and a GP or midwife can refer individuals to the local women’s health physiotherapy team. This treatment may include advice on:
- Daily activities;
- Back care/lifting; and
- An abdominal exercise programme.
If deemed appropriate, a physiotherapist may also provide an abdominal support (elasticated tubular bandage) to wear (around the stomach and low back) during the day until the individual regains some muscular control. This double-layered elasticated material provides some gentle support to the stomach. It may also stimulate and encourage the deeper stomach muscles to work as individuals go about their day to day activities. This may, therefore, be worn while performing the exercises. It can also be worn for more demanding activities, such as housework, pushing the pram and longer walks. Anything more than very light lifting/pushing should be avoided for at least three months.
A small study by Acharry and Kutty (2015) suggests that abdominal exercise with bracing can reduce diastasis recti among postpartum women.
A study by Keeler et al. (2012) looked at the intervention techniques used by physical therapists to address diastasis recti. The study noted that all of the 296 respondents incorporated therapeutic exercise into their plan of care, such as general transverse abdominis (TA) training (89.2%), TA training with functional activities (82.8%) and the Noble technique[16] (62.5%). 59% of the physical therapists used manual therapy techniques and 81.2% used therapeutic modalities. The average number of visits per week was 1.56. The most common length of treatment was 4-6 weeks. 69% of the respondents reported a success rate of 41% to 100%.
10.3 Exercises
The following exercises, both despite of and because of the research outlined in this article, are often recommended to help build abdominal strength, which may or may not help reduce the size of diastasis recti (Liao, 2012).
- Transversus Abdominis: Take a breath in, and then as you breathe out gently draw in your abdominal muscles below your belly button (imagine you are taking in a notch in a low slung belt). Hold this for several seconds whilst breathing normally. Repeat 5-10 times resting between each pull-in. Try to do this exercise several times a day sitting, side-lying or standing. They work with the pelvic floor, so you could do them together. This is likely to be the first exercise a physiotherapist will prescribe, and they will check your progress and monitor the gap between the muscles before giving you other abdominal exercises to practice. The physiotherapist may also fit you with some elasticated abdominal support in order to encourage the linea alba to recover.
- The Abdominal Hollowing Exercise:
 Begin doing this exercise in a comfortable position. If pregnant avoid lying flat on your back. Place your hands on your lower stomach (below your belly button) and as you breathe out, draw in your lower stomach muscles away from your hands and towards your spine. Hold for up to 10 seconds and repeat 10 times, 3 times a day or as often as you can. Make sure that you are not holding your breath.
Begin doing this exercise in a comfortable position. If pregnant avoid lying flat on your back. Place your hands on your lower stomach (below your belly button) and as you breathe out, draw in your lower stomach muscles away from your hands and towards your spine. Hold for up to 10 seconds and repeat 10 times, 3 times a day or as often as you can. Make sure that you are not holding your breath. - Pelvic Tilting:
 Lie with your head on the pillow, knees bent and shoulder length apart. This exercise works the muscles across your lower stomach which supports your back and pelvis. Hollow your abdomen and flatten your back into the bed as your pelvis tilts. Breathe normally. Hold the position for 3-4 seconds. Repeat this up to 10 times, 3 times a day, or as often as you can.
Lie with your head on the pillow, knees bent and shoulder length apart. This exercise works the muscles across your lower stomach which supports your back and pelvis. Hollow your abdomen and flatten your back into the bed as your pelvis tilts. Breathe normally. Hold the position for 3-4 seconds. Repeat this up to 10 times, 3 times a day, or as often as you can. - Pelvic Floor Muscle/Exercises:
 The pelvic floor is like a hammock/sling of muscles suspended from inside the front of your pelvis to the coccyx. There are deep and superficial layers and fast and slow acting fibres. They work with the deep abdominal muscles (transversus abdominis) so when you work your pelvic floor the tansversus abdominis muscles also work. Imagine that you are trying to stop yourself passing wind or urine. Squeeze and lift these pelvic floor muscles, closing and drawing up the back then front passage. Gradually increase the hold time and the number of repetitions until you can hold the squeeze for 10 seconds and repeat 10 times. In addition, tighten them as quickly as you can, then relax immediately and repeat for up to 10 times. Each time you exercise, the muscles become stronger and more supportive. You should also contract them before lifting and coughing.
The pelvic floor is like a hammock/sling of muscles suspended from inside the front of your pelvis to the coccyx. There are deep and superficial layers and fast and slow acting fibres. They work with the deep abdominal muscles (transversus abdominis) so when you work your pelvic floor the tansversus abdominis muscles also work. Imagine that you are trying to stop yourself passing wind or urine. Squeeze and lift these pelvic floor muscles, closing and drawing up the back then front passage. Gradually increase the hold time and the number of repetitions until you can hold the squeeze for 10 seconds and repeat 10 times. In addition, tighten them as quickly as you can, then relax immediately and repeat for up to 10 times. Each time you exercise, the muscles become stronger and more supportive. You should also contract them before lifting and coughing. - Core Contraction: In a seated position, place both hands on the abdominal muscles. Take small controlled breaths. Slowly contract the abdominal muscles, pulling them straight back towards the spine. Hold the contraction for 30 seconds, while maintaining the controlled breathing. Complete 10 repetitions (Liao, 2012).
- Seated Squeeze: Again in a seated position, place one hand above the belly button, and the other below the belly button. With controlled breaths, with a mid-way starting point, pull the abdominals back toward the spine, hold for 2 seconds and return to the mid-way point. Complete 100 repetitions (Liao, 2012).
- Head Lift: In a lying down position, knees bent at 90° angle, feet flat, slowly lift the head, chin toward your chest, (concentrate on isolation of the abdominals to prevent hip-flexors from being engaged), slowly contract abdominals toward floor, hold for 2 seconds, lower head to starting position for 2 seconds. Complete 10 repetitions (Liao, 2012).
- Upright Press-up (or Push-up): A stand-up press-up against the wall, with feet together arms-length away from wall, place hands flat against the wall, contract abdominal muscles toward spine, lean body towards wall, with elbows bent downward close to body, pull abdominal muscles in further, with controlled breathing. Release muscles as you push back to starting position. Complete 20 repetitions (Liao, 2012).
- Squat against the Wall: Also known as a Seated Squat, stand with back against the wall, feet out in front of body, slowly lower body to a seated position so knees are bent at a 90° angle, contracting abs toward spine as you raise body back to standing position. Optionally, this exercise can also be done using an exercise ball placed against the wall and your lower back. Complete 20 repetitions (Liao, 2012).
- Squat with Squeeze: A variation to the ‘Squat against the Wall’ is to place a small resistance ball between the knees, and squeeze the ball as you lower your body to the seated position. Complete 20 repetitions (Liao, 2012).
It is also noted that inappropriate exercises, for example crunches, can increase the degree of diastasis recti separation. All corrective exercises should be in the form of pulling in of the abdominal muscles rather than a pushing of them outwards. Consultation with physiotherapist or appropriately qualified fitness professional is recommended for correct exercise routines (Liao, 2012).
In addition to the above exercises, a study by Engelhardt (1988) concluded that the ‘quadruped’ position yielded the most effective results. A quadruped position is defined as a human whose body weight is supported by both arms as well as both legs. In this position, the subject would start with a flat back, then slowly tilt the head down, and arch the back, contracting the abdominal muscles towards the spine, holding this position for 5 seconds, then releasing back to starting position. Complete 2 sets of 10 repetitions (Engelhardt, 1988).
In a study by Emanuelsson (2014, p.40) “The thirty patients in the training group were followed-up after three months. Twenty-six of these were not satisfied with the outcome of the training programme and were offered surgery.” Emanuelsson (2014, p.45) went on to state “Consequently, these data indicate that physical training does not seem to meet patients’ expectations as they continue to have pain and bulging of the abdominal wall. We further conclude that muscular strength is improved by physical training but that constant physical training is required to maintain a long-lasting result.” Finally, Emanuelsson (2014) concluded that training can improve several of the symptoms witnessed by individuals, but residual pain and patient perception of an instable abdominal wall can remain resulting in dissatisfaction.
Lo et al. (1991) suggest that appropriately modified exercise in early postpartum period can hasten recovery and may reduce the probability of recurrence. Recovery can be enhanced through a regime of appropriate exercise prior to and during pregnancy.
10.4 Surgical
Most, if not all, NHS trusts and clinical commissioning groups (CCGs) do not routinely authorise surgery for diastasis recti and state that surgery should be avoided unless extreme symptoms present. Repair is mostly done due to cosmetic reasons (Hickey et al., 2011; Akram & Matzen, 2014).
However, in extreme cases, diastasis recti is corrected during the cosmetic surgery procedure known as an abdominoplasty (commonly referred to as the ‘Tummy Tuck’) by creating a plication or folding of the linea alba and suturing together. This creates a tighter abdominal wall.
In 2011, Hickey and colleagues conducted a review to examine whether diastasis recti should be repaired and tried to establish if the inherent co-morbidity associated with surgical correction outweighed the benefits derived. They found seven studies that reported high patient satisfaction after surgery and that progressive techniques had resulted in risk reduction with no associated surgical mortality. However, they did report a number of complications:
- Seroma (build-up of bodily fluids), the most common complication;
- Haematomas (a mass of usually clotted blood that forms in a tissue, organ, or body space as a result of a broken blood vessel);
- Minor skin necrosis (death of living tissue);
- Wound infections;
- Dehiscence (the parting of the sutured lips of a surgical wound);
- Post-operative pain;
- Nerve damage; and
- Recurrence (return of symptoms of a disease after a remission), the rate of which may be as high as 40%.
Emanuelsson (2014) suggests that surgical repair of diastasis recti can improve symptoms and general health at the 1-year follow-up.
The general consensus is that women should consider a surgical repair of their abdominal wall for diastasis recti if:
- They are at least one year postpartum;
- They have finished having children;
- They have tried a core exercise programme that specifically targets training the synchronicity of the abdominal muscles and be convinced that their core ‘muscles’ are working well; and
- In spite of good abdominal muscle function, they note that they cannot generate tension in the midline of their abdomen (linea alba) when they do a short head and neck curl-up task.
10.4.1 Abdominoplasty
This surgical technique is suitable for patients who require functional restoration and/or aesthetic rejuvenation of the abdominal wall. Surgery aims to restore a healthy anatomy and strengthen the abdominal wall. As muscle separation usually occurs alongside other concerns such as skin laxity, the repair of diastasis recti is generally performed as part of an abdominoplasty.
During surgery, the rectus abdominis muscles are brought together while shortening and reinforcing the midline. This manoeuvre also repositions the corset-muscles in the flanks, improving both definition and waistline contours. Hernias are corrected as part of this procedure.
Due to the physiological and hormonal changes in the postpartum period, it is generally recommended that a patient waits for 6-9 months after childbirth before undertaking surgical treatment. In brief, an abdominoplasty can:
- Restore and tighten the musculature;
- Repair diastasis recti;
- Correct hernias;
- Remove skin laxity/stretch marks; and/or
- Decrease thickness of the subcutaneous fat and improve the waistline.
Traditional abdominoplasty techniques address extra-abdominal fat through liposuction and resection, and correction of diastasis recti and abdominal wall hernia(s) through direct fascial repair including plication of the linea alba (Repta & Hunstad, 2009). Intra-abdominal fat can be a significant source of abdominal protrusion, but it is not addressed in traditional abdominoplasty techniques. The last potential source of abdominal wall protrusion is global myofascial laxity. Abdominoplasty patients with significant abdominal protrusion and relatively little intra- and extra-abdominal fat frequently have abdominal wall laxity that is much greater than the degree of diastasis recti present (Repta & Hunstad, 2009). Deferring plication or plicating only sufficiently to decrease the width of the linea alba frequently results in inadequate correction of abdominal wall laxity and the persistence of abdominal wall protrusion. Hunstad & Repta (2008) prefer to use the term myofascial plication to better describe the process of global myofascial laxity correction. They suggest the technique is similar to standard diastasis recti plication; however, plication involves imbricating a wider portion of the anterior rectus sheath as determined by preoperative assessment and intraoperative estimation with the patient under muscular relaxation. The process of myofascial plication shortens the width of the anterior rectus sheath and in turn pulls the paired linea semilunaris toward midline, resulting in re-approximation of the medial edges of the rectus muscles (Hunstad & Repta, 2008). This entire process results in overall tightening of the abdominal wall as a myofascial unit. The frequency and significance of global myofascial laxity are often under-appreciated in the process of abdominal wall tightening for the abdominoplasty patient (Hunstad & Repta, 2008).
10.4.2 Other Surgical Treatments
Besides abdominoplasty there are a number of other surgical treatments, which include:
- In adult females, a laparoscopic Venetian blind technique can be used for plication of the recti (Palanivelu et al., 2009)
- Repair with a retromuscular mesh: “Retromuscular inlay of a lightweight polypropylene mesh (BARD™Soft Mesh)” (Emanuelsson, 2014, p.22). (Nahas, F.X., Augusto, S.M. & Ghelfond, C. (2001) Nylon versus Polydioxanone in the Correction of Rectus Diastasis. Plastic and Reconstructive Surgery. 107(3), pp.700-706.). Excision of the thinned fascia and placement of a mesh prosthesis alleviate the deformity (Norton, 2003).
- General surgeons repair diastasis recti and incisional hernias using a retromuscular mesh, widely undermining the rectus muscles.
- The wide dissection required when inserting a mesh could result in higher risks for bleeding, postoperative pain, injury of supporting nerves to the rectus muscles as well as postoperative seroma, compared to the Quill technique.
- On the other hand, one would expect mesh repair to provide more long-lasting stability of the abdominal wall.
- Double layer plication of the anterior rectus sheath using an absorbable self-retaining barbed suture (Quill™ Self-Retaining System) (Emanuelsson, 2014, p.22). (QuillTM self-retaining system (SRS) comprised of dyed PD0 (polydioxanone) synthetic absorbable surgical suture material. Instructions for use. Reading, PA: Angiotech. 2007–2009.).
- The self-retaining double-row technology is thought to improve the repair by vertical anchoring of the rectus aponeurosis.
- These anchors might reduce the risk of cutting through the fibres of the rectus aponeurosis compared to conventional polydioxanone sutures
Emanuelsson’s (2014) study revealed no statistical difference in terms of early complications between the two surgical techniques. Seroma occurred equally in both groups despite the extent of undermining and implantation of foreign material in the mesh group. The very first patient repaired with the Quill technique developed a recurrence within one month but this must be “considered a technical failure” (Emanuelsson, 2014, p.43).
10.5 Abdominal Supports
Postpartum abdominal (or belly) binding has been traditional practice in many parts of the world for generations. This is the process of wrapping or binding your mid-section to draw the split abdominal muscles back together. As such abdominal binding:
- May ‘hold you in’;
- Should provide support to the midline, and
- Should provide support to the lower back.
However, a number of experts suggest that wearing an abdominal support will not strengthen or tighten the muscles, although it could help quicken the healing process. Strengthening or tightening of the muscles can only be done through specific exercises or, failing that, surgery. An abdominal support will not magically return your six-pack. A study by El-Mekawy et al. (2013, p.48) would suggest otherwise, stating “…the use of post-natal belt in group (A) also produces a statistically significant increase in abdominal muscles strength (Peak torque, maximum repetition total work and average power) and a statistical significant decrease in waist circumference…”
One of the problems of a wearing a brace is that it can result in a patient’s over-reliance on the brace, thereby reducing the opportunity to retrain the abdominal muscles. That said, there are situations when a brace is necessary, especially if a patient cannot properly contract their abdominal muscles.
For instance, if they cannot engage their transverse abdominis muscles then they will likely compensate and use the rectus abdominis. Incorrect usage of the rectus abdominis will reinforce and even continue to split the diastasis recti. Once the patient can contract and use the transverse abdominis properly then it is important to stop the patient using the brace to prevent over-reliance. A small study by Acharry and Kutty (2015) suggests that abdominal exercise with bracing can reduce diastasis recti among postpartum women.
A number of binding retailers will inform the reader that their particular product is specifically designed to treat diastasis recti. However, any material which can be wrapped around the midline can be suitable for the task of ‘holding you in’ and providing support; and won’t cost £40. Other common terms for abdominal supports include:
- Diastasis recti splint;
- Binder;
- Belt;
- Corset;
- Girdle;
- Support belt;
- Wrap; and
- Waist clincher.
Some individuals will also use Kinesio tape, invented by a Japanese chiropractor Dr Kenzo Kase in the 1970s, which it is claimed can alleviate pain, reduce inflammation, relax muscles, enhance performance and help with rehabilitation as well as supporting muscles during a sporting event.
However, there has not been conclusive scientific or medical evidence to confirm the effectiveness of the tape. A review of evidence (Williams et al., 2012) from 10 research papers for Kinesio tape to treat and prevent sports injuries concluded the following:
- No clinically important results were found to support the tape’s use for pain relief;
- There were inconsistent range-of-motion results;
- Seven outcomes relating to strength were beneficial;
- The tape had some substantial effects on muscle activity, but it was not clear whether these changes were beneficial or harmful; and
- The study concluded there was little quality evidence to support the use of Kinesio tape over other types of elastic taping to manage or prevent sports injuries.
Other studies have come to similar conclusions (González-Iglesias et al., 2009; Mostafavifar eet al., 2012; Saavedra-Hernández et al., 2012). González-Iglesias et al. (2009) concluded that although patients exhibited statistically significant improvements immediately following application of the Kinesio Tape and at a 24-hour follow-up, the improvements in pain and cervical range of motion were small and may not be clinically meaningful.
The UK website has a research section which provides a wide range of research papers for public consumption (158 case studies and 83 randomised control trials as of January 2015). And, unusually, the website provides a summary column indicating whether the paper provides a positive (clinical benefit of Kinesio tape) or negative (no clinical benefit) outcome.
Some experts have suggested there may be a psychological (or placebo) effect in using the tape, with athletes believing it will be helpful, rather than a physical effect. However, never underestimate the power of placebo.
10.6 Tupler Technique
The Tupler Technique, devised by Julie Tupler, is a 4 step programme, the goal of which is to “…heal the weakened connective tissue that joins your outermost abdominal muscles.” (Diastasis Rehab, 2014). The 4 steps are:
- The Tupler Technique seated and back-lying exercises;
- Splinting the separated muscles (with a Diastasis Rehab Splint®);
- Strengthening and learning how to use the transverse abdominis muscle; and
- Getting up and down correctly.
The programme is delivered over an 18-week period, with the Tupler Technique being introduced in week 6.
Julie Tupler is a Registered Nurse, Certified Childbirth Educator and Certified Personal Trainer. She developed the Maternal Fitness Programme in 1990 and for over 20 years has been teaching and developing the Tupler Technique Programme for the treatment of diastasis recti for women, men and children.
The website states the programme is the only research-based exercise programme proven to effectively treat a diastasis recti. However, this research by Chiarello et al., (2005) only comprised a total of 18 pregnant women (8 women participating in the Tupler Technique abdominal exercise programme and 10 non‐exercising women) and utilised a quasi-experimental post-test design.
 Quasi-experimental designs get their name because they are not true experimental designs, where patients are randomly assigned to treatment and control groups (Cook & Campbell, 1979). In quasi-experimental designs, outcomes may only be measured at the end of the study (rather than at the beginning and end), there may not be a control group, or patients may be assigned to the control and treatment groups by methods other than randomisation. However, quasi-experimental studies can sometimes provide a more natural, generalisable environment that better establishes effectiveness (as opposed to efficacy); although the post-test only design is the simplest and probably weakest quasi-experimental design (Cook & Campbell, 1979).
Quasi-experimental designs get their name because they are not true experimental designs, where patients are randomly assigned to treatment and control groups (Cook & Campbell, 1979). In quasi-experimental designs, outcomes may only be measured at the end of the study (rather than at the beginning and end), there may not be a control group, or patients may be assigned to the control and treatment groups by methods other than randomisation. However, quasi-experimental studies can sometimes provide a more natural, generalisable environment that better establishes effectiveness (as opposed to efficacy); although the post-test only design is the simplest and probably weakest quasi-experimental design (Cook & Campbell, 1979).
Due to the lack of a pre-test, it is impossible to determine whether the two groups of women where comparable prior to the start of the research. Lack of random assignment, a major weakness (Harris et al., 2006), and internal validity issues Shadish et al. (2002) are causes for concern in this type of study design. The website also provides a number of webpages displaying a variety of statistics, however, there is no control group statistics only intervention group statistics (the website states individuals serve as their own controls!). Although diastasis recti may take up to 1-year to resolve in post-partum women, in most cases diastasis recti usually heals on its own; so it is somewhat problematic to discern causality.
The research conducted by Chiarello et al. (2005) and cited by the website is one of the eight studies (18/336 women) included in the systematic review of the evidence by Benjamin et al. (2014) that found that exercise may or may not reduce the size of the gap in pregnant or postpartum women (see Section 10.0). However, also remember the small study by Acharry and Kutty (2015) that suggested that abdominal exercise with bracing can reduce diastasis recti among postpartum women.
The most distinct difference between the Tupler Technique and the MuTu System (discussed next) is the use of binding.
10.7 MuTu System
The MuTu System, devised by Wendy Powell, “is for women who want their bodies to look, feel and function better after having a baby.” (MuTu System, 2015). It is described as a step by step series of highly instructive online coaching videos and workouts (with PDFs) over a period of 12 weeks. It combines tummy flattening, core strengthening, pelvic floor restoring expertise, as well as an eating plan and low impact but high intensive workouts to help women tone, shape, drop fat and lose weight.
The MuTu Focus programme is described as an alternative option designed especially for women who want to avoid all intensive exercise, whether out of personal preference or for medical or other reasons. The website states the the MuTu Focus programme is just the parts of the main 12-week programme that deal purely with restoring core and pelvic floor function, narrowing a diastasis recti through alignment adjustments and gentle reconnection and strengthening of the core muscles.
Although the site has the endorsement of a number of physiotherapist’s, there is no reference to research to back up the claims on the effectiveness or efficacy of the programme.
Wendy Powell qualified as a personal trainer in 2001, having spent the previous ten years working in media and advertising in London (UK). She devised the MuTu System in 2010.
Margie Langweg, an ACE-Certified Personal Trainer and advocate for the MuTu System, wrote the following on her blog (2014):
“So, I was more than slightly disappointed when I started the program only to learn that it was just a bunch of stretches. Really, that’s the program…stretches with a few exercises thrown in. I later learned, however, that these stretches and simple exercises are vital to healing your core.”
Margie, who has used by the MuTu System and the Tupler Technique, provides a somewhat unbalanced (i.e. slightly biased) view in her appraisal of the two methods. For example, noting the cost of books associated with the Tupler Technique whilst neglecting to mention the cost of MuTu materials. In a reply to one enquiry, Margie states (2014): “Do not complete any program that requires a binder or wrap.”
A more balanced review of the two methods has been written by Edith Erickson (2015), which the reader is encouraged to investigate: http://619healthandfitness.com/workouts/diastasis-recti/tupler-vs-mutu/.
11.0 What is the Prognosis or Outlook?
- In most cases, diastasis recti usually heals on its own.
- However, for post-partum women it may take up to a year for their body to recover from having a baby; so do not give up with the advice and exercises.
- Occasionally a marked gap will persist that causes symptoms and may require surgery. Your physiotherapist should be able to answer any questions you may have regarding this and initiate a referral as required.
- Exercise may help improve the condition.
- Umbilical hernia may occur in some cases.
- If pain is present, surgery may be needed.
- In infants, the diastasis will resolve as abdominal musculature develops further (Uffman, 2012).
Research by Lo and colleagues (1999) suggests that earlier recovery may also be associated with:
- Lower parity;
- Singleton birth;
- Weight gain under 35 pounds;
- Birth of baby less than 3600 grams;
- Increased activity levels before, during, and after pregnancy; and
- Severity of the diastasis recti.
12.0 Personal Notes
- At no point during either of her pregnancies (before, during or after childbirth) did my wife receive any advice/information on diastasis recti, from a physiotherapist, midwife, doctor or health visitor. This is despite having a diastasis recti, albeit now within the ‘normal range’.
- Also, despite being a (military and civilian) qualified fitness instructor, I had little knowledge on this condition prior to writing this article.
- It pains me to think that I may have prescribed/did prescribe inappropriate exercises to some of my clients resulting from a lack of knowledge.
- This article is based on work commissioned by my wife for an audit she was conducting at her GP practice.
13.0 Summary
There are a myriad of websites and blogs which display a variety of views/representations on the condition known as diastasis recti. There is also an increasing database of research, but there is still more to be understood. Despite its prevalence, especially in pregnant and postpartum women, it still surprises people when they acquire the condition.
- Lifestyle choices can impact on the development of and healing process for diastasis recti.
- If you exercise in a gym or outdoor setting make sure you are working with a personal trainer/fitness instructor who knows what diastasis recti is and can provide appropriate exercises.
- An abdominal band will aid in ‘holding you in’ and relieving pressure on the midline, which could quicken the healing process. It will not magically return your six-pack.
- Avoid heavy lifting.
- The best time to begin core strengthening is before you get pregnant, if you don’t already have an abdominal separation!
- All corrective exercises should be in the form of pulling in of the abdominal muscles rather than a pushing of them outwards.
Definitions
- [1] The main musculature of the abdomen is held together at the anterior midline by a long, triangular structure called the linea alba. The linea alba’s insertion is at the xiphoid process of the sternum and extends downward to the pubis (Brauman, 2008).
- [2] Any of the broad flat sheets of dense fibrous collagenous connective tissue that cover, invest, and form the terminations and attachments of various muscles.
- 3] A small sac containing tissue that protrudes through an opening in the muscles of the abdominal wall. The main cause of hernia formation is an abdominal wall weakness or defect.
- [4] A sheet of connective tissue (as an aponeurosis) covering or binding together body structures, e.g. muscles.
- [5] Inward curvature of the spine. A certain degree of lordosis is normal in the lumber and cervical regions of the spine: loss of this is a sign of ankylosing spondylitis (inflammation of the synovial joints of the backbone). Exaggerated lordosis may occur in adolescence, through faulty posture or as a result of disease affecting the vertebrae and spinal muscles. Kyphosis is the excessive outward curvature of the spine, causing hunching of the back.
- [6] The arcuate line of the abdomen, linea semicircularis or Douglas’ line is a horizontal line that demarcates the lower limit of the posterior layer of the rectus sheath. It is also where the inferior epigastric vessels perforate the rectus abdominis.
- [7] In anatomy, an arcuate line is any structure that is curvilinear (consisting of or bounded by curved lines).
- [8] A diseased state or symptom.
- [9] I.e. death.
- [10] A negative aftereffect.
- [11] Women who have had a baby.
- [12] Bottom of the breast bone.
- [13] Tapering toward each end.
- [14] The smooth transparent serous membrane that lines the cavity of the abdomen of a mammal.
- [15] A fold of peritoneum connecting or supporting abdominal structures (as the stomach and liver).
- [16] Developed by Elizabeth Noble, a pioneer in women’s health physical therapy.
14.0 References
Acharry, N. & Kutty, R.K. (2015) Abdominal Exercise with Bracing, A Therapeutic Efficacy in Reducing Diastasis-Recti Among Postpartal Females. International Journal of Physiotherapy and Research. 3(2), pp.999-1005. DOI: 10.16965/ijpr.2015.122.
AHC Media (2014) Abdominal Wall Hernias in Adults: Diagnosis and Management. Emergency Medicine Reports. Available from World Wide Web: http://www.ahcmedia.com/articles/17077-abdominal-wall-hernias-in-adults-diagnosis-and-management. [Accessed: 10 May, 2015].
Akram, J. & Matzen, S.H. (2014) Rectus Abdominis Diastasis. Journal of Plastic Surgery and Hand Surgery. 48(3), pp.163-169. doi:10.3109/2000656X.2013.859145.
http://informahealthcare.com/doi/abs/10.3109/2000656X.2013.859145
Axer, H., Keyserlingk, D.G. & Prescher, A. (2001) Collagen Fibers in Linea Alba and Rectus Sheaths. I. General Scheme and Morphological Aspects. The Journal of Surgical Research. 96(1), pp.127-134.
Beer, G.M., Schuster, A., Seifert, B., Manestar, M., Mihic-Probst, D. & Weber, S.A. (2009) The Normal Width of the Linea Alba in Nulliparous Women. Clinical Anatomy. 22(6), pp.706-711.
Benjamin, D.R., van de Water, A.T.M. & Peiris, C.L. (2014) Effects of Exercise on Diastasis of the Rectus Abdominis Muscle in the Antenatal and Postnatal Periods: A Systematic Review. Physiotherapy. 100(1), pp.1-8. DOI: 10.1016/j.physio.2013.08.005).
http://www.csp.org.uk/physio-journal/100/1/effects-exercise-diastasis-rectus-abdominis-muscle-antenatal-postnatal-periods-
http://www.crd.york.ac.uk/crdweb/ShowRecord.asp?ID=12013069654#.VVpknfm6eM8
Boissonnault, J.S. & Blaschak, M.J. (1988) Incidence of Diastasis Recti Abdominis during the Childbearing Years. Physical Therapy. 68(7), pp.1082-1086.
Boxer, S. & Jones, S. (1997) Inter-rater Reliability of Rectus Abdominis Diastasis Measruement using Dial Calipers. Australia Journal of Physiotherapy. 43(2), pp.109-114.
Brauman, D. (2008) Diastasis Recti: Clinical Anatomy. Plastic and Reconstructive Surgery. 122(5), pp.1564-1569. http://journals.lww.com/plasreconsurg/Abstract/2008/11000/Diastasis_Recti__Clinical_Anatomy.30.aspx
Brown, L.J. & Miller, L.T. (2005) Pediatrics. London: Lippincott, Williams & Wilkins.
Bursch, S.G. (1987) Interrater Reliability of Diastasis Recti Abdominis Measurement. Physical Therapy. 67(7), pp.1077-1079.
Candido, G., Lo, T. & Janssen, P.A. (2005) Risk Factors for Diastasis of the Recti Abdominis. Journal of the Association of Chartered Physiotherapists for Women’s Health. 97, pp.49-54.
Chiarello, C.M. & McAuley, J.A. (2013) Concurrent Validity of Calipers and Ultrasound Imaging to Measure Interrecti Distance. Journal of Orthopaedic Sports and Physical Therapy. 43(7), pp.495-503.
Chiarello, C.M., Falzone, L.A., McCastin, K.E., Patel, M.N. & Ulery, K.R. (2005) The Effects of an Exercise Program on Diastasis Recti Abdominis in Pregnant Women. Journal of Women’s Health and Physical Therapy. 29(1), pp.11.
Coldron, Y., Stokes, M.J., Newham, D.J. & Cook, K. (2008) Postpartum Characteristics of Rectus Abdominis on Ultrasound Imaging. Manual Therapy. 13(2), pp.112-121.
Cook, T.D. & Campbell, D.T. (1979) Quasi-Experimentation: Design and Analysis Issues for Field Settings. Boston: Houghton Mifflin.
De’Ath, H.D.I., Lovegrove, R.E., Javid, M., Peter, N., Magee, T.R. & Galland, R.B. (2010) An Assessment of Between-Recti Distance and Divarication in Patients with and without Abdominal Aortic Aneurysm. Annals of the Royal College of Surgeons of England. 92(7), pp.591-594. DOI: 10.1308/003588410X12771863937089
El-Mekawy, H.S., Eldeeb, A.M., El- Lythy, M.A. & El-Begawy, A.F. (2013) Effect of Abdominal Exercises versus Abdominal Supporting Belt on Post-Partum Abdominal Efficiency and Rectus Separation. International Journal of Medical, Health, Biomedical and Pharmaceutical Engineering. 7(1), pp.44-48.
Emanuelsson, P. (2014) Alternatives in the Treatment of Abdominal Rectus Muscle Diastasis: An Evaluation. Thesis. Available from World Wide Web: https://openarchive.ki.se/xmlui/handle/10616/42245. [Accessed: 08 May, 2015].
Engelhardt, L. (1988) Comparison of Two Abdominal Exercises on the Reduction of the Diastasis Recti Abdominis of Postpartum Women. ProQuest Dissertations and Theses. UMI Dissertations Publishing. [Accessed: 08 May, 2015].
Erickson, E. (2015) The Tupler Technique VS The MuTu System Review. Available from World Wide Web: http://619healthandfitness.com/workouts/diastasis-recti/tupler-vs-mutu/. [Accessed: 19 May, 2015].
Gilleard, W.L. & Brown, J.M.M. (1996) Structure and Function of the Abdominal Muscles in Primigravid Subjects during Pregnancy and the Immediate Postbirth Period. American Physical Therapy Association. 76(7), pp.750-762.
González-Iglesias, J., Fernández-de-Las-Peñas, C., Cleland, J.A., Huijbregts, P. & Del Rosario Gutiérrez-Vega, M. (2009) Short-term Effects of Cervical Kinesio Taping on Pain and Cervical Range of Motion in Patients with Acute Whiplash Injury: A Randomized Clinical Trial. The Journal of Orthopaedic and Sports Physical Therapy. 39(7), pp.515-521.
Harms, R.W. (2014) Why Do Abdominal Muscles Sometimes Separate during Pregnancy? Available from World Wide Web: http://www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/expert-answers/diastasis-recti/faq-20057825. [Accessed: 07 May, 2015].
Harris, A.D., McGregor, J.C., Perencevich, E.N., Furuno, J.P., Zhu, J., Peterson, D.E. & Finkelstein, J. (2006) The Use and Interpretation of Quasi-Experimental Studies in Medical Informatics. Journal of the American Medical Informatics Association. 13(1), pp.16-23. DOI: 10.1197/jamia.M1749.
Hickey, F., Finch, J.G. & Khanna, A. (2011) A Systematic Review of the Outcomes of Correction of Diastasis of the Recti. Hernia. 15(6), pp.607-614.
Hsia, M. & Jones, S. (2000) Natural Resolution of Rectus Abdominis Diastasis. Two
Single Case Studies. Australia Journal of Physiotherapy. 46(4), pp.301-307.
http://www.kinesiotaping.co.uk/research/index.jsp [Accessed: 20 May, 2015].
Hunstad, J.P. & Repta, R. (2008) The Atlas of Abdominoplasty. London: Saunders.
Keeler, J., Albrecht, M., Eberhardt, L., Horn, L., Donnelly, C. & Lowe, D. (2012) Diastasis Recti Abdominis. Journal of Women’s Health Physical Therapy. 36(3), pp.131-142. DOI: 10.1097/JWH.0b013e318276f35f.
Kuber, S. (2013) Hernia Surgery Simplified. New York: JP Medical Ltd.
Langweg, M. (2014) MuTu System vs. Tupler Technique: Healing Diastasis Recti. Available from World Wide Web: http://lucyfitpt.blogspot.co.uk/2014/03/Mutu-tupler-diastasis.html. [Accessed: 19 May, 2015].
Liao, S. (2012) 15 Minutes and You’re Done: Crunch-free Abs. Available from World Wide Web: http://www.realsimple.com/health/fitness-exercise/workouts/ab-workout. [Accessed: 18 May, 2015].
Liaw, L.J., Hsu, M.J., Liao, C.F., Liu, M.F. & Hsu, A.T. (2011) The Relationships between Inter-recti Distance Measured by Ultrasound Imaging and Abdominal Muscle Function in Postpartum Women: A 6-month Follow-up Study. The Journal of Orthopaedic and Sports Physical Therapy. 41(6), pp.435-443. http://www.ncbi.nlm.nih.gov/pubmed/21289454
Lo, T., Candido, G. & Janssen, P. (1999) Diastasis of the Recti Abdominis in Pregnancy: Risk Factors and Treatment. Physiotherapy Canada. 51(1), pp.32-37.
Lockwood, T. (1998) Rectus Muscle Diastasis in Men: Primary Indication for Endoscopically Assisted Abdominoplasty. Plastic and Reconstructive Surgery. 101(6), pp.1685-1691.
Mendes, A., Nahas, F.X., Veiga, D.F., Mendes, F.V., Figueiras, R.G., Gomes,
H.C., et al. (2007) Ultrasonography for Measuring Rectus Abdominis Muscles Diastasis. Acta Cirurgica Brasileira/Sociedade Brasileira para Desenvolvimento Pesquisa em Cirurgia. 22(3), pp.182-186.
Moore, K.L. & Agur, A.M.R. (1995) Essential Clinical Anatomy. London: Lippincott, Williams & Wilkins.
Mostafavifar, M., Wertz, J. & Borchers, J. (2012) A Systematic Review of the Effectiveness of Kinesio Taping for Musculoskeletal Injury. The Physician and Sports Medicine. 40(4), pp.33-40.
Mota P.G.F., Pascoal, A.G.B.A., Sancho, F. & Bo, K. (2012) Test-retest and Intrarater Reliability of 2-dimensional Ultrasound Measurements of Distance between Rectus Abdominis in Women. The Journal of Orthopaedic and Sports Physical Therapy. 42(11), pp.940-946.
Mota, P.G.F., Pascoal, A.G.B.A., Carita, A.I.A.D. & Bo, K. (2015) Prevalence and Risk Factors of Diastasis Recti Abdominis from Late Pregnancy to 6 Months Postpartum, and Relationship with Lumbo-pelvic Pain. Manual Therapy Journal. 20(1), pp.200-205.
http://www.manualtherapyjournal.com/article/S1356-689X(14)00181-7/abstract
http://www.manualtherapyjournal.com/article/S1356-689X(14)00181-7/fulltext
Mota, P.G.F., Pascoal, A.G.B.A., Sancho, F., Carita, A.I.A.D. & Bo, K. (2013) Reliability of the Inter-rectus Distance Measured by Palpation: Comparison of Palpation and Ultrasound Measurements. Manual Therapy Journal. 18(4), pp.294-298. http://www.ncbi.nlm.nih.gov/pubmed/23298825
Nahas, F.X. (2001) An Aesthetic Classification of the Abdomen based on the Myoaponeurotic Layer. Plastic and Reconstructive Surgery. 108(6), pp.1787-1795; discussion 96-7.
Norton, J.A. (2003) Essential Practice of Surgery: Basic Science and Clinical Evidence. New York: Springer-Verlag.
Palanivelu, C., Rangarajan, M., Jategaonkar, P., Amar, V., Gokul, K. & Srikanth, B. (2009) Laparoscopic Repair of Diastasis Recti using the ‘Venetian Blinds Technique of Plication with Prosthetic Reinforcement: A Retrospective Study. Hernia. 13(3), pp.287-292.
Parker, M.A., Millar, A.L. & Dugan, S.A. (2009) Diastasis Rectus Abdominis and Lumbo-Pelvic Pain and Dysfunction-Are They Related? Journal of Women’s Heath Physical Therapy. 33, pp.15-22.
Pascoal, A.G.B.A., Dionisio, S., Cordeiro, F. & Mota, P.G.F. (2014) Inter-rectus Distance in Postpartum Women can be Reduced by Isometric Contraction of the Abdominal Muscles: A Preliminary Case-control Study. Physiotherapy. 100, pp.344-348.
Potter, H.M., Randall, H.F. & Strauss, G.R. (1997) Effect of Pregnancy and Motherhood on Trunk Muscle Strength: An Examination of Isokinetic Trunk Strength at 24 Weeks Postpartum. In: 10th Biennial Conference of the Manipulative Physiotherapists Association of Australia. Victoria: Manipulative Physiotherapists Association of Australia. pp.151-152.
Ranney, B. (1990) Diastasis Recti and Umbilical Hernia Causes, Recognition and Repair. South Dakota Journal of Medicine. 43(10), pp.5-8.
Rath, A.M., Attali, P., Dumas, J.L., Goldlust, D., Zhang, J. & Chevrel, J.P. (1996) The Abdominal Linea Alba: An Anatomo-radiologic and Biomechanical Study. Surgical and Radiological Anatomy: SRA. 18(4), pp.281-288.
Repta, R. & Hunstad, J.P. (2009) Diastasis Recti: Clinical Anatomy. Plastic and Reconstructive Surgery. 123(6), pp.1885. http://journals.lww.com/plasreconsurg/fulltext/2009/06000/diastasis_recti__clinical_anatomy.40.aspx
Saavedra-Hernández, M., Castro-Sánchez, A.M., Arroyo-Morales, M., Cleland, J.A., Lara-Palomo, I.C. & Fernández-de-Las-Peñas, C. (2012) Short-term Effects of Kinesio Taping versus Cervical Thrust Manipulation in Patients with Mechanical Neck Pain: A Randomized Clinical Trial. The Journal of Orthopaedic and Sports Physical Therapy. 42(8), pp.724-730.
Shadish, W.R., Cook, T.D. & Campbell, D.T. (2002) Experimental and Quasi-experimental Designs for Generalized Causal Inference. Boston: Houghton Mifflin.
Sheppard, S. (1996) The Role of Transversus Abdominus in Postpartum Correction of Gross Divarication Recti. Manual Therapy Journal. 1(X), pp.214-216.
Speed, C. (2004) Low Back Pain. BMJ 2004;328:1119. DOI: http://dx.doi.org/10.1136/bmj.328.7448.1119
Spitznagle, T.M., Leong, F.C. & Van Dillen, L.R. (2007) Prevalence of Diastasis Recti Abdominis in a Urogynecological Patient Population. International Urogynecology Journal of Pelvic Floor Dysfunction. 18(3), pp.321-328.
http://libra.msra.cn/Publication/29183757/prevalence-of-diastasis-recti-abdominis-in-a-urogynecological-patient-population
Stevens, A.B. (2013) Hernias. Critical Decisions in Emergency Medicine. 27(9), pp.2-8.
Uffman, C. (2012) Surgically Correctable Hernias in Children. Available from World Wide Web: https://www.cookchildrens.org/SiteCollectionDocuments/HealthCareProfessionals/CCPNsurgicallycorrectablehernias_nov2012.pdf. [Accessed: 18 May, 2015].
Volkan, T., Cagda, C., Esengul, T. & Umit, K. (2011) Prevalence of Diastasis Recti Abdominis in the Population of Young Multiparous Adults in Turkey. Ginekol Pol. 82, pp.817-821.
Vox Health (2015) Diastasis Recti. Available from World Wide Web: http://voxhealth.org/voxhealth/VHdiaginfo.php?diag=Diastasis%20recti. [Accessed: 20 May, 2015].
Williams, S., Whatman, C., Hume, P.A. & Sheerin, K. (2012) Kinesio Taping in Treatment and Prevention of Sports Injuries: A Meta-analysis of the Evidence for its Effectiveness. Sports Medicine (Auckland, NZ). 42(2), pp.153-164.
Zaoutis, L.B. & Chiang, V.W. (2007) Comprehensive Pediatric Hospital Medicine. New York: Elsevier Health Sciences.

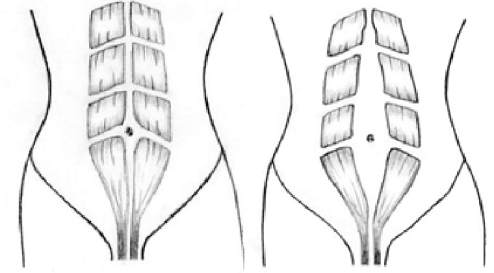
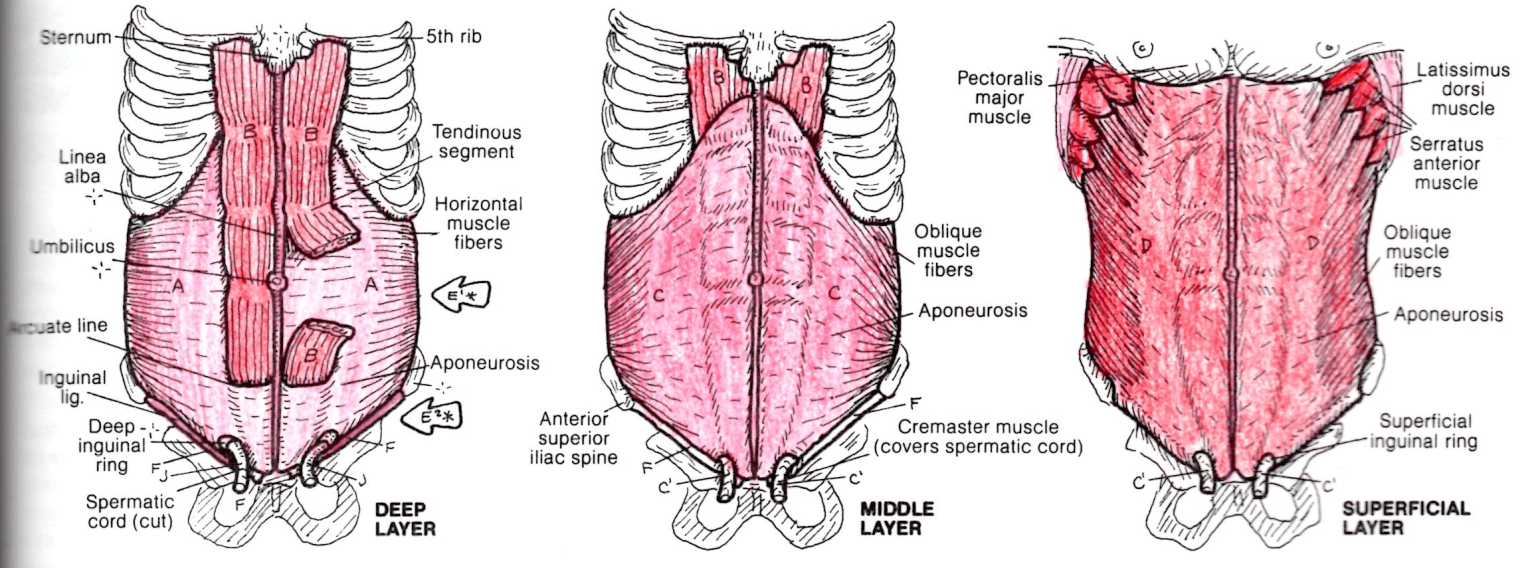
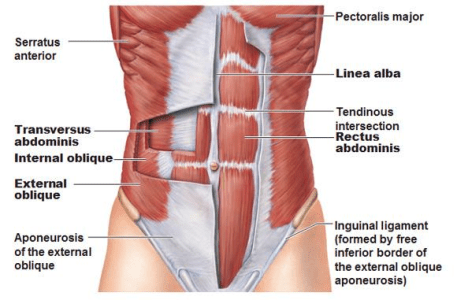



Andrew, thank you for this excellent article! I had my baby 6 years ago, and was not able to straigthen up all the way for several days afterwards. Then I did lots of baby lifting and even had a front carrier. There’s still a 1 finger-width separation, but the linea is quite deep and weak, no pain. Can’t wait to do back stretches and twists again, without risking further harm. I agree that there’s a need to be more informed about this condition for both women who are preparing for pregnancy and health professionals.
LikeLike
i have severe diastis, is it ok, to swim and ride my bike? i am 64 yr. old. very weak core. have some my pelvic pushes forward
LikeLike
Hi Adella,
1. I would require more information to give a meaningful, tailored response.
2. Severe DR? What are the dimensions?
3. In general, it would probably be ok to ride a bicycle, typically on flat ground.
4. In general, it would probably be ok to swim.
5. It may be advisable to seek guidance from a qualified physiotherapist (with experience in treating DRs specifically) to gain tailored advice/treatment.
LikeLike
Hello, I’m writing a bachelor’s dissertation about physiotherapy in diastasis recti. Your article is really helpful, I will use it in my work. I would like to know who is the author of this. I need it to put this information in my bibliography.
LikeLike
Hi Dominika,
Citation: Marshall, A. (2015) Diastasis Recti: An Overview. Available from World Wide Web: https://bootcampmilitaryfitnessinstitute.com/injury/diastasis-recti-an-overview/. [Accessed: 29 November, 2016].
LikeLike
Thank you!
LikeLike
Hi
Excellent write up. I am a male 51 yo, one question, does having this stop me working on my upper body strength, bench presses , curl bars and dumb bells, several sites mention using weights (without overdoing them) to assist but it seems slightly contradictory and can I do push ups if wearing a brace/corset
Bill
LikeLike
Hi Bill,
Simple Answer: Q1, No; Q2, Yes.
Longer Answer: 1) Firstly a caveat: it is difficult to provide specific, tailored advice to a client you haven’t seen (e.g. what is size of the DR, does it give pain etc). 2) Regarding weightlifting, the general advice is against exercising with heavy weights – with heavy being contextual to the individual. For some a 60kg bench press is heavy and for others it is light. 3) Regarding press-ups with a brace/corset, it depends on your DR. One press-up might give pain and discomfort, whereas you may complete 500 press-ups without any pain or discomfort.
If you would like a more ‘private’ (and detailed) conversation then email me at andrewm@bootcampmilitaryfitnessinstitute.com
LikeLike
Thank you for this! I had a bad diastasis recti of 11cm after my first baby in 2012, had I not asked the midwife why my stomach was so strange, it wouldn’t have been picked up on. I also could hardly find any information regarding it. No-one seems to know for certain why some people seem more prone to develop it than others, it would definitely be useful if more research was conducted. Pilates has been very useful in developing my core strength and helping to close the gap. Have had 2 more babies since, again with the separation post-birth. I’m certain that there are many women walking around undiagnosed, just having become accustomed to their ‘mummy tummy’. As a nurse I would love to see more information out there to raise women’s awareness of this condition.
LikeLike
Can you join the army if you have diastasis recti or have had it in the past?
LikeLike
Hi Amanda,
Short Answer: No, but the medical professional at your medical examination would have the final say.
Longer Answer: My wife has a DR and it does not affect her functionally nor is it painful. All, if not most, of the ‘fitness experts’ with a knowledge of DR will inform you that conducting normal sit-ups is a no-no, however, as a member of the military you will have to do them. If your DR is: within the accepted norms (i.e. 0.1-3.0cm); no pain; no functional disability; and you can do normal sit-ups, then you will likely be ok. If you have not already done so (through your own training regime), try some normal sit-ups (5-10) and progress to completing the 2-minute sit-up test (50) and note how your body reacts.
LikeLike